Join the TriWest Healthcare Alliance Network
Are you interested in joining TriWest’s network of medical professionals to care for military families and Veterans? Visit our TRICARE Provider Contracting Q&A page for more details or read on and then submit the online Join Our Network form. TriWest’s provider contracting team looks forward to working with you.
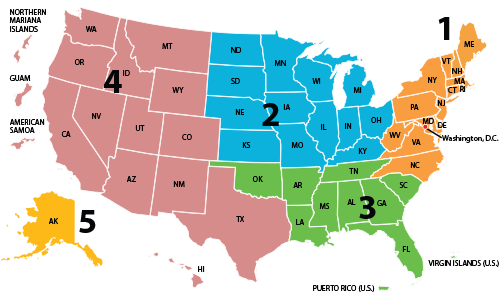
TriWest Provider Network Serving both DOD and VA

Who TriWest Serves
Patient eligibility for VA CCN and enrolled TRICARE is different.
- VA CCN — This is for eligible Veterans as defined by VA.
- TRICARE — This is for enrolled active duty service members, active duty family members, National Guard and Reserve members and their family members, military retirees and their family members, survivors, and certain former spouses.
Subscribe for TriWest Network News
To stay updated on TRICARE and VA CCN provider-related news, subscribe to TriWest’s eNewsletter, Provider Pulse.